You’ll agree that becoming a mom is scary.
You’re now responsible for a whole tiny little human. That includes making lots of important decisions for them.
Within the first few days after birth, you’ll be asked to make a whopping 14 life-changing medical decisions for your baby. You may already be aware of some of these decisions, but do you know all your options?
It’s vital that you are informed about these choices before your baby arrives. Otherwise, you need to make a quick decision during the pain of labor or after the exhaustion of delivery.
If you don’t make a decision, your caregivers will likely make one for you.
This informed choice guide is here to help you make the best decisions for your baby. What’s right for your family may not be right for other families. We’ll discuss all your options and the possible consequences.
This guide is massive and has a lot to take in. I recommend you bookmark or pin it for later. That way you can read it in bite-sized chunks, without information overload.
Pin for Later
14 Life-Changing Decisions to Make for Baby
1. Cord Clamping
Once your baby is born, the cord is clamped and cut to separate your baby from the placenta. This immediately stops any blood flow between you and baby. If everything is straightforward, you can decide how long you want to wait until the cord is clamped and cut. You have three options to choose from.
Early Cord Clamping
Usually, this is done by your doctor or midwife within 2 minutes of your baby being born. This is the option most caregivers will take unless you state a preference. There are a few reasons why early cord clamping is beneficial. If you want to collect stem cells from the cord (see next point), you may get more with early clamping.
Your doctor may also need to clamp and cut early, for resus, if your baby’s heart rate is very low after birth. This may be particularly true after a difficult birth or emergency cesarean delivery.
If you are at high risk of PPH (post-partum hemorrhage) and start bleeding heavily, the cord will need to be cut quickly. This is so they can administer the essential medicine to stop and assess the cause of your bleeding.
Your caregiver may also need to take cord blood samples for specific antibody or thyroid testing. You should be aware of a plan for this during pregnancy and discuss with your doctor or midwife.
Delayed Cord Clamping
This involves waiting around 5 minutes until after birth to cut clamp and cut the cord. It offers a few more benefits to your baby.
Immediately after birth the cord still contains about 30% of your baby’s total blood volume. By waiting to clamp, all this blood flows into your baby’s system. This is thought to protect your baby against breathing difficulties and anemia, especially if they are premature.
If your baby is struggling to breathe, but their heart rate is ok, delayed cord clamping can help keep them oxygenated. It’s best to discuss this with your caregiver first as they may not be comfortable with delaying resuscitation.
Delayed cord clamping is still possible even if you are having an active third stage (assisted). If you opt for this choice the best time to clamp and cut is 4 minutes after birth.
Studies have found that delayed cord clamping is not linked to increase the rates of newborn jaundice.
Lotus Birth
This option is when you do not clamp or cut the cord after birth. Baby stays attached to the umbilical cord and placenta until it dries up and falls off a few days after birth. You need to make sure you have somewhere to store the placenta alongside baby before it detaches.
A special placenta cloth, salt and herb rub will help the placenta dry out and prevent it smelling before it falls off.
Reasons to have a lotus birth include a spiritual connection to your baby; encouraging mom to take it easy and to discourage baby from being ‘passed around’ visitors.
A lotus birth will not be an option for you if your placenta does not detach after a vaginal birth. You will need to go to a theatre to have it manually removed.
2. Cord Blood Banking
The blood in your baby’s umbilical cord is known to be rich in stem cells. These cells can be collected and used in medical treatment. It’s similar to a bone marrow donation, which is also rich in stem cells.
Collecting this umbilical cord blood is not harmful to your baby. It’s taken from areas of clamped cord between where it is cut from baby and attached to the placenta. Cord blood banking is still possible if you opt to have delayed cord clamping.
You have three options when it comes to cord blood banking.
Cord Blood Donation
This is like a baby blood drive. Just as you would donate to a blood bank. Any blood extracted from your baby’s cord is then screened, processed and available for public use by suitable matches.
It’s entirely free to donate cord blood. Apart from telling your caregivers, there is little you need to do, apart from giving a blood sample for screening purposes.
Donating to a public bank gives a larger stock to choose from, creating more potential matched for seriously ill patients.
It’s important to remember that it’s highly unlikely a donation will be available for you or your baby to use in the future. It may also be rejected as a donation in the screening process or used for research purposes instead.
Private Cord Blood Banking
You can pay a private company to retrieve your baby’s cord blood and store it for future use. You have full rights to the sample and have access to use it at any point. The cord blood can also be used for any suitable family members and not just your baby.
If you have a strong family history of a particular disease or have a rare blood type, it’s good health insurance to have.
Private cord banking costs around $2000 for the initial collection, then $100-$200 per year for storage.
No Donation
If you don’t choose any type of cord blood banking, the cord will just be discarded as medical waste. That is unless you request to take the placenta home with you.
Related: Cord Blood Banking Prep in Pregnancy
3. Holding Baby
If all is well at the delivery, you can choose how to hold your baby after they are born. You can opt to have your baby placed straight onto you or swaddled first. The Apgar score can be assessed at 1 and 5 minutes, whichever method you choose. Let’s explore each option.
Skin to Skin
This is when your baby is placed directly on your bare chest. Baby is dried with a towel on you, then a clean blanket put over you both. Ideally, skin to skin should last for at least 1 hour after birth.
Skin to Skin is highly encouraged as it is known to regulate baby’s breathing and temperature. It can also help speed up placenta delivery, reduce bleeding and encourage baby to start breastfeeding. It is particularly helpful if your baby is born slightly premature but well enough to stay with you.
The touch, smell and sight of each other promotes bonding, attachment, and your baby’s transition into the world.
Make sure baby is kept without a hat or diaper during this time for best results. They are not needed and will disrupt the attachment between you and baby.
If you need stitches, you can still hold baby while they do the procedure.
Usually, skin to skin is only interrupted if there is an emergency with you or baby need to be taken to NICU for extra support.
Swaddled baby
This option is better if you would prefer your baby to be cleaned up with a diaper on before holding them. This the standard procedure for a cesarean birth as you will still be on the operating table.
You may also feel sick, tired, shaky or too medicated to hold your baby correctly after birth. Your birth partner can opt for skin to skin or support baby next to you.
Your religion may not promote skin to skin contact at birth, let your caregiver know this before delivery.
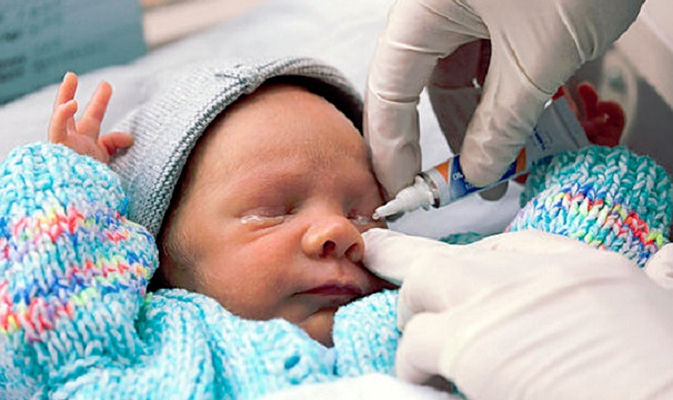
4. Eye Ointment
Some hospitals routinely offer babies to have eye ointment within one hour after birth. The eye goop is actually an antibiotic treatment such as erythromycin, tetracycline or silver nitrate. The idea is to cleanse the eyes to prevent any infection usually associated with sexually transmitted disease (STD). Some states require you to give it by law, please research what
Some states require all babies have eye ointment by law. Please research your own state’s laws are on this topic.
Choosing the ointment
This is only essential if you have tested positive for an STD such as chlamydia, gonorrhea or herpes. Any infection left untreated after a vaginal delivery can cause your baby to go blind. Getting tested in the third trimester will ensure your baby receives the correct treatment for any known disease you have.
You may also opt for the ointment as protection if you have been treated for a previous STD but not an active one.
If you need to administer due to state law, wait until at least two hours after birth. Request the least irritating agent such as tetracycline.
No Ointment
If you have a cesarean birth, there is no need for ointment, regardless of known infection. This is because your baby will not pass through the birth canal.
Prophylactic use of eye ointment without known infection is actually harmful to your baby. It can cause eye irritation and blurring which disrupts the crucial skin-to-skin bonding. Your baby may even be allergic to the ointment, but you won’t know until it’s given.
The good bacteria in your birth canal helps your baby to develop a strong immune system. Giving unnecessary antibiotics can disrupt this process and cause future problems for your baby’s health.
If your state law requires you to administer, but you decline, you may be charged a penalty or threatened with Child Protection Services (CPS). You may want to discuss this with your local CPS to fully understand what this would involve, as it may be pure intimidation tactics.
5. Vitamin K
Vitamin K is used by the body to help with blood clotting. It’s an essential vitamin to stop bleeding. Newborn babies are born with low levels of vitamin K, compared to adults.
Adults get most Vitamin K from food, which your baby won’t get until they start on solids.
This ‘deficiency’ is thought to put newborns at higher risk of severe internal bleeding known as or Vitamin K Deficiency Bleeding (VKDB).
The medical solution is to offer a synthetic dose of vitamin K to your baby after birth. There are three options you can take with Vitamin K.
Vitamin K Injection
This is the most popular option offered to parents. It’s an intra-muscular shot of vitamin K given in the leg. It’s quick to administer, and your baby only needs to be given once.
This method is highly recommended if your baby has had a traumatic delivery, long or speedy labor or born with cuts or bruising. Specific medication may also interfere with Vitamin K production. In these cases, your baby is at higher risk of internal bleeding. Premature or low birth weight babies may also have smaller stores and may benefit from an extra boost of vitamin K.
Mature breast milk contains smaller amounts of vitamin K than fortified formula. If your baby is having problems feeding they may benefit from a vitamin K shot.
Oral Vitamin K
If you want your baby to have vitamin K but you are put off by an injection, opt for an oral dose. This needs to be given three times: one treatment at birth, once on day 3-7 and one dose at 6 weeks.
An oral dose means the vitamin k is administered via the gut, just like the body naturally would. Three doses are given to ensure your baby gets the same dose as a shot. Although it’s difficult to tell how much they will absorb through the gut.
No Vitamin K
You may choose to opt out of giving vitamin K to your baby altogether. The question is why human babies have evolved to be born with low levels of vitamin K?
The dose given to a term baby is usually 1mg which is 20,000 times your baby’s natural volume. This will be adjusted for a low birth weight or premature baby. Administering this much vitamin K can cause your baby to develop jaundice.
If everything was straightforward with birth, your baby is at a lower risk of being affected by VKDB. Although it’s impossible to tell which babies will be affected by VKDB.
If you opt out of the Vitamin K shot, start to increase your own intake of Vitamin K rich foods in pregnancy. Once your baby is born, give them as much colostrum as possible as it’s extremely rich in vitamin K.
6. Supplementation
There may be situations that arise where you are recommended to supplement your breastfed baby. These medical reasons may indicate that your baby needs further nutrients to help them grow and develop. Let’s look at your options for supplementation.
Breast Milk Supplement
A baby who is having difficulty or cannot breastfeed can still be given breast milk. They can be fed by cup, spoon or tube instead. It’s mainly recommended for babies who are in NICU.
This is also an excellent method for sleepy babies or if you have sore nipples. Nutrients can be added to the breast milk to restore any deficiencies your baby may have.
You will need to learn to express breastmilk either by hand or using a breast pump. This helps to keep your milk supply high by removing milk from your breasts. You can then try baby at the breast at a later date.
The Simply Breastfeeding Course is a great resource for new moms. Cindy and Jana created a chapter on how to hand express. In fact, they recommend it as a vital skill to learn and succeed at breastfeeding, and I totally agree.
Donor Milk
If you are unable to produce any breast milk, you may opt for donor breast milk. It’s a useful option if you want your baby to have breastmilk, but they cannot use your own. Medications, infectious disease or medical conditions may mean your own breast milk may be harmful to your baby.
Click here for a list of Donor Milk Banks in the USA and Canada.
Formula Supplement
Formula supplementation should only be used for under these circumstances:
- Your preference of supplement
- Baby cannot use any type of breast milk due to rare metabolic disease
- Donor milk is not available or declined
- You are unable to express enough milk for baby’s needs
Giving formula supplement to a breastfed baby is known to cause problems with nursing. It can interrupt your baby’s gut bacteria and is associated with low milk supply and higher levels of quitting.
The benefit of using formula milk is that there is a constant supply available. It is also calorific and can promote quick weight gain in babies who are not gaining weight with breast milk.
7. Hepatitis B Vaccine
Hepatitis B is a liver disease that can pass from mom to baby. The Center for Disease Control and Prevention recommends all babies have the Hep B vaccine before they are discharged from the hospital.
If your baby contracts Hepatitis B as a baby, it puts them at a 25% increased risk of chronic liver disease.
Having the Vaccine
The best way to protect your baby from Hep B is to give your baby the vaccine. It’s given as a shot in their arm or leg. Your baby will then need 2-3 more injections within the first 6 months, as boosters.
Even if you don’t pass it on at birth, your baby can contract Hep B from other infected adults or children. Hepatitis B can be contacted from blood, open sores or being bitten.
You can opt to delay the first vaccine until your baby is around 8 weeks old.
No Vaccine
The most likely way your baby will contract Hep B is from vaginal fluid during birth. If you are not a Hepatitis B carrier, you cannot pass it onto them. If you are sure your baby will not come into contact with a Hep B affected adult or child, there is no need for the vaccine.
As with any vaccine, there may be side effects which range in severity. You may want to avoid any risk that vaccines present to your baby’s immune and nervous system.
8. Pacifier
A pacifier is an artificial teat you can give to baby for them to suckle on. There are a lot of pros and cons to using a pacifier.
Using a Pacifier
The sucking motion of a pacifier is well known to soothe most babies quickly. They are particularly useful if your baby wants to suck all the time, even if they are not hungry. There is also an active link between using a pacifier and a lower risk of SIDS.
Breaking a pacifier habit is easier than if your baby decides to be a thumb sucker.
Avoiding a Pacifier
The biggest concern with pacifiers is missing your babies feeding cues. These are really important when breastfeeding, as it can affect your milk supply. As the sucking motion from a teat is different to that of breastfeeding, it can cause teat confusion for your baby.
Pacifier use is linked to an increased risk of ear infections in babies and young children. You may also have trouble parting baby from their pacifier. Long-term use of a pacifier can lead to speech and dental problems for your baby.
Related: How to Lower Your Baby’s Risk of SIDS
9. Hospital Stay
Once you’ve given birth to your baby, you’ll usually be moved to a maternity ward or private room to recover until discharge. If your baby doesn’t need to be taken to the NICU, you can choose where you want your baby to stay. These are your options.
The Nursery
This means your baby will be kept in a separate room from you overnight, alongside other babies. The nursery is staffed by a nurse or midwife who takes care of your baby for you. They will even monitor baby for feeding cues and give them formula or bring them to you for a breastfeed.
This gives you and your partner the opportunity to rest after delivery. You can care baby during the day, then get rest overnight in-between feeds.
If you are worried about security, ask your hospital what the procedures are regarding the hospital nursery.
Rooming In
If you don’t want to be parted from your baby, opt to ‘room in.’ This means keeping your baby alongside you until you are discharged. It’s a great option if you are breastfeeding, as it makes skin to skin and reading feeding cues so much easier.
It’s an excellent way for you to have full control over what happens to your baby. When your baby is always with you, nobody can perform procedures, administer meds, give pacifiers or supplements without you knowing.
If you become exhausted, you can always ask for your baby to be taken to the nursery for a few hours to get some rest.
10. First Bath
Birth is quite a messy process. Your baby will probably be covered in a greasy vernix, blood, amniotic fluid and even poop. It’s only natural you want to clean your mucky baby. You may want to re-consider how soon you give your baby a bath.
Early Bathing
Your baby can have a bath within the first few hours to clean them up. You may prefer this to get lovely newborn photos and pass your baby to your visitors. Your religion may require you bathe baby within a set time frame.
As a first-time parent, a bathing demo can be helpful. This will usually need to be done when your nurse or midwife is free.
Delayed Bathing
Waiting until your baby is at 24-48 hours before bathing is a WHO recommendation. The reason is that the vernix on your baby’s skin is antibacterial and helps their immune system. This is especially important if your baby is born by cesarean and not exposed to good bacteria in your birth canal.
The stress of a bath can cause your baby’s blood sugars to drop as they use up vital energy. In the first 24 hours, your baby will work on regulating their body temperature. It’s better to bath once they are less likely to have a significant drop in temperature. Make sure you have a lot of skin to skin with your baby to help them maintain a proper temperature.
Related: 10 Reason Delayed Bathing Can Improve Your Postpartum
11. Hearing Test
Your baby will be offered a hearing screen test shortly after birth. This test is designed to identify if your baby has hearing loss as early as possible. This means you can get treatment, support, and advice as soon as possible.
Having the Hearing Test
The test is called the automated otoacoustic emission (AOAE) test. It involves placing an earpiece on your baby’s ear and transmitting soft clicking sounds. The equipment will detect how your baby responds to these sounds. It is not painful for your baby. However, it may make them unsettled.
You get a pass or a fail result straight away. This doesn’t mean your baby does or does not have hearing loss. A fail result means referral to an audiologist for further testing.
This test is highly recommended if there is a higher risk of hearing loss or your baby has spent more than 48 hours in NICU. The test cost around $30-$50 to perform.
No Hearing Test
The AOAE is a screening test, not a diagnostic test. That means your baby can still have some hearing loss even if they get a pass on the initial test.
You may prefer to observe your baby carefully for any signs of hearing loss as they grow.
It can be quite tricky to get your baby at a right time when they are settled enough to test. Some hospitals may even recommend mild sedation. If the test is done too early, gunk from birth can cause a false result. If you are likely to worry about these results, you may want to avoid the stress.
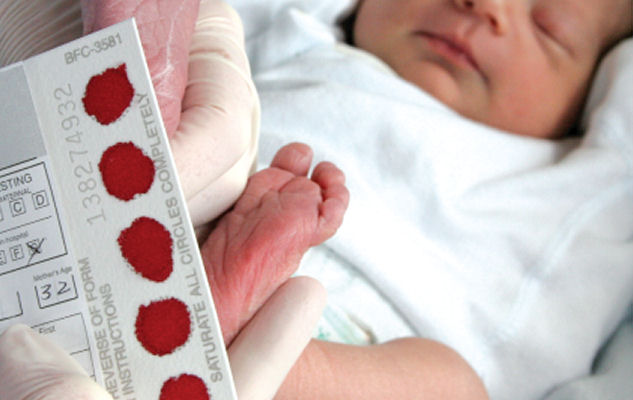
12. Guthrie Test
This is a screening test offered to your baby. It’s also known as the newborn blood spot or heel prick test. A blood sample is taken from baby and analyzed for various metabolic diseases. This test gives you an early diagnosis of the tested diseases and can help with early treatment.
Choosing the Test
The first test will usually be carried out soon after birth. Your baby’s heel will be pricked to draw blood. The blood drops are collected on an individual filter paper and sent to labs to test for the various diseases. The test may be repeated just before you are discharged, to compare the samples.
You may need to wait a few weeks for the results of the test. You will usually only be contacted if your baby tests positive for any condition. Further tests will be required to make a proper diagnosis of any condition.
Early recognition makes some of these rare diseases completely treatable. It may also save your baby’s life or prevent severe mental disability. This test is highly recommended if you have a family history of any of the diseases tested for.
No Testing
You may find it unnecessary to put your baby through a painful test for rare diseases. Even more so if your baby is low risk.
It is also possible you may get a false positive result. This means you get a positive result even when your baby does not have a condition. This may lead to you unnecessarily paying for further investigation or stopping breastfeeding on medical advice. A false diagnosis may also cause worry and stress for your family.
You may prefer to observe your baby closely and report any signs of health conditions. You can also delay testing for up to 12 months, although some screens may be time sensitive.
13. Circumcision
If you have a boy, then you may be asked about circumcision. This is a surgical procedure to remove the foreskin from your baby’s penis. The procedure cannot be done without permission and a signed consent.
Routine circumcision is not recommended by the AAP. Unless there is a medical reason, circumcision is a cosmetic preference. It’s a hugely debated topic, so make sure you are fully informed of all the risks and benefits of this procedure.
Choosing to Circumcise
Circumcision had been linked to fewer urine infections, STDs, yeast infections and cancer rates.
You may be recommended to circumcise your baby if your baby has medical problems related to the foreskin.
Your religion or culture may prefer your baby to be circumcised as routine. You will need to arrange your own ceremonial procedure if you opt to have the circumcision outwith a hospital.
If you choose to circumcise for cosmetic purposes, please make yourself fully aware of the potential risks and complications that can occur from the procedure. Never choose it as an option due to family pressure or because ‘everyone else does.’
Leaving Intact
You may wonder why males are born with a foreskin if it doesn’t serve a purpose. Painful and unnecessary surgery for your baby may lead to lifelong complications with their penis.
You put your baby at increased risk of bleeding, pain, infection, and amputation of part of the penis. Many of the benefits of circumcision can be prevented with proper hygiene and safe sex practices.
Other possible future complications for your baby include reduced sensation, permanent tenderness, deformity, further surgery, and urinary or sexual health complications.
14. Choosing a Baby Doctor
The best time to start looking for a doctor for your baby is in your third trimester. Ask family, friends, co-workers or your pregnancy caregivers for recommendations. By the time you deliver you can have a list of potential doctors to choose from.
Contact the doctor to make sure they are accepting patients and will take your health insurance. You might then want to interview them and choose the best.
If you do not pick a doctor by the time you deliver, your hospital will assign you a pediatrician.
You’ll need to choose someone you are comfortable seeing. Your child will see a doctor for wellness checks throughout their childhood, or more when they get ill.
Pediatrician
Pediatricians are doctors who specialize in childhood medicine. They are the experts when it comes to dealing with baby and child illness or conditions. A pediatrician will look after your baby from birth until they are 21, then they will need to switch doctors.
If your baby has a known medical condition, they are better with specialized care. They will often be assigned to a consultant who specializes in your child’s specific condition.
Family Practitioner
A family practitioner is a doctor of general medicine. They are trained to recognize and treat general disease and ailments. Once your family practitioner diagnoses a condition that requires specialist treatment your child will need a referral to a pediatric specialist.
A family practitioner can look after your baby from birth to old age. They also have a better idea of the whole family’s overall health and medical history.
Summary
Now to have a good idea of the decisions you’ll have to make for your baby after they are born. A lot of these you will already feel strongly about. Other choices may require a bit more thought or discussion with your partner.
Remember to write your preferences down in your birth plan. This way your caregivers will know your choices for baby. It can help them prepare or make them aware of your religious or cultural needs during labor and delivery.